About Us
Our Story
As a healthcare executive, I’ve become all too familiar with the challenges of our healthcare system. While the emergence of technology has promised to address health disparities, improve patient outcomes, relieve professional burden, and deliver cost savings, it has failed to deliver on its potential. Like many, I have spent most of my career on the sidelines discussing problems and theoretical solutions from a comfortable office while witnessing the prevalence of chronic diseases grow and health inequities widen in our country.
When I first met RPM-One Co-Founder, Matt Willert, we discussed the limitations of wearable technology and barriers to widespread adoption. Primarily, poor data integrity (limiting trust), lack of specificity and clinical workflows (limiting utility) and high cost (limiting accessibility). Based on my experience in wearable technology as a Physiologist and data scientist, and Matt’s success in operations, we began assessing the feasibility of a business model that would allow us to provide a solution to those who need it most. We spent months on end evaluating each and every business decision, working closely with patients and healthcare professionals, based on improving accessibility and clinical utility, not making more money.

“As with any true startup, there has been disagreements and pivots, but we have never wavered from our shared mission of solving global inequities through purposeful applications of technology. By providing no cost medical devices to patients, interoperable software, advanced data analytics to improve efficiency and quality of care delivery, and on-demand clinical staffing, RPM-One is a critical component in addressing health inequity. ”
-Kevin Longoria, Chief Executive Officer

COMPANY OVERVIEW
RPM-One, Inc. is a software and technology provider operating in the industry of remote physiologic monitoring (RPM). The RPM-One fully managed solution provides a no-cost medical device to medically underserved patients, predictive algorithms to detect and prioritize care (Digital Triage™), interoperable software, and on-demand clinical staffing for real-time care coordination. Our business model aligns the interest of health systems, medical professionals, patients, and payers through a value-based solution that addresses health inequity, improves patient outcomes, decreases readmissions, and results in cost savings.
THE PROBLEM
Despite the validated benefits of remote physiologic monitoring (RPM) to improve health equity, health systems have struggled to implement the complex clinical and operational infrastructure necessary to support novel care delivery. Third-party solutions remain costly and fragmented, thereby limiting access and clinical utility.
Hardware
Cost Prohibitive, Compliance Issues, Racial Bias in Collection Methodology
Software
IT/Implementation Challenges, Inefficient Care Management, Interoperability
Clinical Monitoring
Staff burden & shortages
Health Inequity
Health inequity limits underserved populations’ access to affordable, high-quality healthcare and results in an avoidable socioeconomic burden that spans society and affects every individual’s potential to achieve health and financial well-being. Unnecessary spending attributable to health inequity is estimated at $320 billion annually and project to surpass $1 trillion annually by 2040. Attributable factors include diminished access to general health services, delayed care, missed diagnosis, and limited access to the latest scientific advancements and preventive services.
There is a disparity in the access to health resources for underserved populations that only technology, when developed with respect to clinical standards and human factors, can address.

RPM-ONE Solution
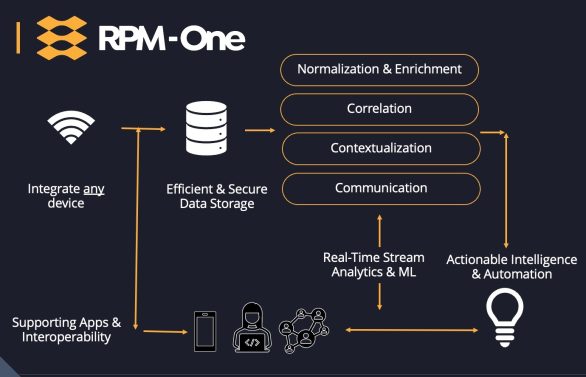
The RPM-One solution is a fully managed remote monitoring program that does not require upfront investment, adoption of new software, or staffing to minimize barriers to adoption.
Our evolutionary system leverages remote monitoring technology, artificial intelligence for clinical decision support and automated administrative tasks, and a diverse workforce of contracted medical professionals, in an ecosystem that aligns the interests of all by making novel care delivery more efficient, cost effective, and accessible.

T.E.C.H. Foundation
The T.E.C.H. Foundation provides equitable access to healthcare technology through strategic deployment of Connected Healthcare Technology Centers (CHTCs) in Medically Underserved Areas (MUAs). The CHTCs provide the base infrastructure of connected, safe, trusted, and secure locations for medically underserved populations to access the highest quality of care from qualified healthcare professionals anywhere in the world. Access to the CHTC and all services are provided at no cost, and do not require identifiable information or insurance documentation to be provided.
The CHTCs are staffed to provide local support to circumvent technological and health literacy barriers and serve as physical locations for third-party organizations to deliver no-cost primary health services, health screening initiatives, and distribution of medical products and services.
